Admission to hospital and delayed discharge can affect people’s mental and physical wellbeing and make them increasingly dependent on support services. Multidisciplinary intermediate care services have a crucial role to play in supporting people to recover and regain independence.
More people are living longer, often with complex or multiple medical conditions, putting increasing pressure on the NHS and social care services. NHS Digital's Health Survey for England found that people aged 80 or over were more than twice as likely to need help with daily activities as people aged 65 to 69. Intermediate care and reablement services can help people, particularly older people, remain independent by:
- providing support and rehabilitation to people at risk of admission to, or who have been in, hospital
- helping make their transfer out of hospital as smooth as possible
- ensuring they don't have to move into residential care until they really need to
- offering short-term support to people living at home who find daily activities difficult.
Intermediate care works. The NHS Benchmarking Network's National Audit of Intermediate Care found that 93% of people receiving these services in 2018 improved or maintained their independence.
NHS Digital's Adult Social Care Outcomes Framework found that 83% of people aged 65 and older who received reablement or rehabilitation services after being discharged from hospital were still at home 91 days later, but there's a lot of variation across the country.
The occupational therapist came around the day after I came out of hospital and put rails up for me and a toilet seat. I felt much safer.
Later in the day a really nice carer with a big smile on his face came in and said he would be coming three times a day for two weeks to help me spruce up, get meals, help me with my medicines and keep the place tidy. I felt more confident immediately and thought - yes - I can manage at home.
NICEimpact adult social care:
Intermediate care is a multidisciplinary service. Home-based intermediate care and reablement take place in people's own homes or care homes. Bed-based intermediate care takes place in hospitals, care homes, nursing homes and standalone intermediate care facilities.
We've produced quick guides for people using intermediate care services and staff delivering them. These are a quick, easy way to access key information from our guidance.
Proportion of people able to stay at home after receiving reablement or rehabilitation services
England
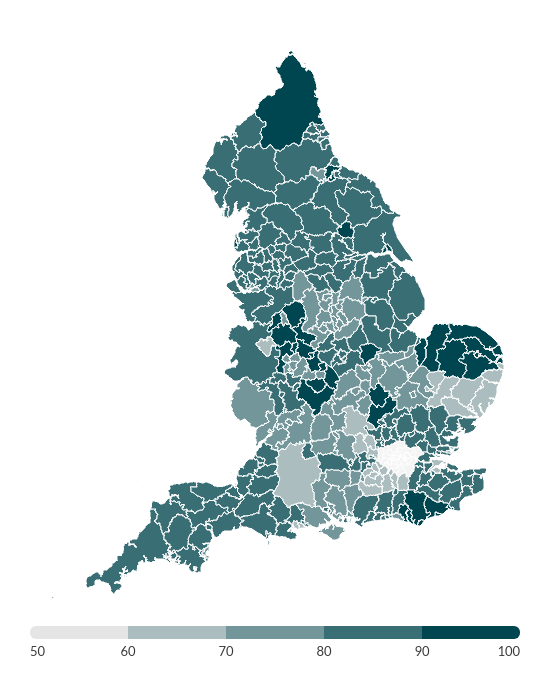
London
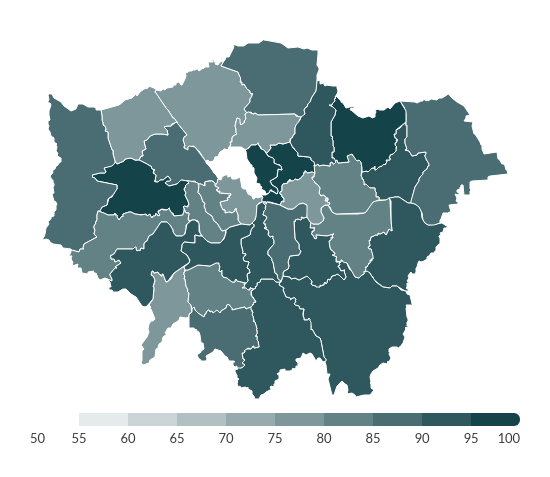
You can download the data sets used to generate these heat maps.
To improve outcomes, NICE's guideline and quality standard set out how people should be referred and assessed for intermediate care including reablement, and how these services should be delivered.
Starting and ending intermediate care
The National Audit of Intermediate Care found that 17% of people who were referred for bed-based intermediate care waited more than 2 days for the service to start in 2018. NICE recommends 2 days as the maximum waiting time for this service because it's likely to be less successful if there's a delay. Only 44% of commissioners reported that they have a local waiting time target in their service specification for bed-based intermediate care.
Almost all people receiving intermediate care or reablement services said they were aware of what they were aiming to achieve and were involved in setting those aims. NICE recommends that people starting intermediate care discuss and agree personalised goals, which is important if they're to regain their confidence and independence.
It's also important that there's a clear plan for what happens when the service ends. NICE says this should be agreed with the person and their family or carers. Most people (93%) receiving home-based intermediate care or reablement said they were given enough notice about when their care from the community team was going to stop. Nearly 9 in 10 people receiving bed-based intermediate care said they were involved in decisions about when they would go home.
Reablement services
The focus of reablement is on helping people relearn how to perform their daily activities, like cooking meals, washing and getting about, after a deterioration in their health or when they have increased support needs. It's a community-based service, usually delivered to people in their own home.
Reablement has the highest proportion of social care staff of all intermediate care services. More than half the people working in it are social care support workers or social workers. Most reablement services provide support for up to 6 weeks and the average duration of service was 31 days in 2018.
The National Audit of Intermediate Care shows how successful reablement is. Eighty-six percent of people completed their package of care and around two-thirds of those had no ongoing homecare needs after receiving the service.
Reablement is often someone's first contact with social services. It's a very important service and everyone should have the opportunity to engage. It's always a pleasure when someone regains independence, often with the use of aids and techniques promoted by the reablement assistants
Commissioning integrated services
The National Audit of Intermediate Care found that more integrated services are being commissioned. In 2017 we recommended that different intermediate care services, such as home-based and bed-based intermediate care, should be delivered in an integrated way. This can make it easier for people to move between services, depending on their changing needs.
More integrated services are now being commissioned
Although there have been improvements in commissioning, many services are not yet delivering care in a fully integrated way. NICE lists some ways of delivering integrated care that services should be working towards. This includes a single point of access and assessment process. This can help make sure that people get the right care and support when they need it.
Most integrated services have multidisciplinary team meetings but a single point of access is less common. Only 37% of commissioners report that there's a single point of access for their whole intermediate care system, so there's more to do in this area.
Since our 2017 guideline was published, a higher proportion of commissioners are commissioning integrated services.
Integrated home-based intermediate care and reablement services
Integrated home-based and bed-based intermediate care services
Most integrated services have improved their delivery of these NICE-recommended components of integrated care
Commissioning an integrated Home First service in Bristol
The city council, clinical commissioning group and community health provider in Bristol helped more people return home from hospital by working together and commissioning an integrated rehabilitation and reablement service. They used NICE guidance on transition between inpatient hospital settings and community or care home settings for adults with social care needs and on intermediate care to help them address local issues.
The health and care partners in Bristol knew they had a higher rate of delayed transfers out of hospital than other areas. They also found that many people who hadn’t previously been known to social care were being transferred from hospital straight into long-term care.
Their new Home First service aims to bring people out of hospital then assess and support them in their own home. Early results are encouraging. The integrated service supported 38 people to go home from hospital in the week before Christmas 2018, one of the busiest times of the year. The separate rehabilitation and reablement services had only been able to support between 20 and 25 people a week.
Improving access to community crisis response services
Crisis response is a community-based service, provided to people in their own home or a care home, which aims to avoid hospital admissions. It usually involves an assessment and may provide short-term interventions. NICE says that services should ensure that the crisis response can be started within 2 hours from receipt of a referral when necessary.
In line with this recommendation, NHS England's Ageing Well Programme seeks to implement a new 2 hour waiting standard for crisis response services by 2023/24. The NHS Long Term Plan highlights that achieving this, through extra investment and productivity reforms in community health services, could free up over a million hospital bed days.
Being able to reference that we used NICE guidance in our design processes and in creating our standard operating procedures gave us the ability to give challenging messages with the backing of NICE credentials. This was particularly helpful when communicating changes with the acute providers.

