The National Rheumatoid Arthritis Society (NRAS) follows best practice, evidence-based standards in all we do. Whilst huge strides have been made in the diagnosis and treatment of Rheumatoid Arthritis (RA), the impact on quality of life can be significant and for many RA remains hard to come to terms with.
NRAS has contributed to NICE Guidelines and Quality Standards since the first RA guideline in 2009. We promote adherence to the Guideline and Standards.
The aim of Right Start is to improve outcomes of the newly diagnosed with RA through a framework of supported self-management resources tailored to individual need. It’s a simple, 4-step process starting with health professionals referring patients to NRAS (consented) online. This enables health professionals to meet their responsibilities against NICE Quality Standard 33, Statement 3, on which they are audited through National Early Inflammatory Arthritis Audit (NEIAA), and improve patient outcomes at the same time.
Right Start outcomes are being evaluated by King’s NHS Trust as part of a quality improvement programme nested with the national audit.
Example
Aims and objectives
We wanted to evidence that in providing the right kind of support to people with RA at the right time, in line with NICE NG100 and QS33, we can improve their self-efficacy and outcomes. This would thereby demonstrate the ‘value’ of NRAS in an evidence-based way.
Being diagnosed with a condition like RA can be a devastating experience, and often people see their life’s dreams and goals disappearing in front of their eyes. Fortunately, today the way in the which the disease is treated, especially if caught early, is dramatically better than the situation many years ago. However, the impact on quality of life is still significant and for many, hard to come to terms with. Anxiety and depression are common co-morbidities especially in early RA, which can be as high as 40%, and there are well documented studies demonstrating this. This can prevent people from being able to self-manage effectively.
From experience, we were confident that if people were given the right support and education at the start of their journey, we could help to reduce feelings of anxiety and depression and improve emotional wellbeing. We are also able to debunk myths and unhelpful health beliefs and encourage and support medicines’ adherence, reinforcing the messages from their clinic visit.
Key points of importance were:
- to link the service directly to the NICE Quality Standard on education and self-management
- rheumatology teams are being audited against these standards
- HCP run, in-hospital educational programmes have dramatically reduced due lack of resources.
- With ‘Right Start’, we are not only providing high quality education and support, but enabling HCPs to meet their obligations under QS 33 – standard 3
- We are enabling HCPs to have confidence they are providing their patients with access to excellent educational and supported self-management resources.
Once referred into the service, NRAS contacts the person to arrange:
- a call (up to 1 hr) with a member of our helpline.
- 1:1 and community peer support
- a tailored package of hard copy information with e-links of interest sent by post
- further follow up available by helpline and individual peer support
Data analysis on the first tranche of patients who have completed Right Start has just started.
Reasons for implementing your project
We know from experience that people with RA who engage with us early in their journey benefit hugely, sometimes in life-changing ways, from the type of expert support and resources we provide. We were equally aware that HCPs, whilst generally aware of us and some of the resources we provide, don’t always understand or value the benefit derived by their patients who do engage with us. We wanted more people to be able to benefit and therefore concluded that we needed to better demonstrate our value in an evidence-based way, so as to enable HCPs to feel even more confident in referring patients to our services.
“I’ve used the helpline a couple of times over the past week or two, I really wanted to say thank you so very much, these early weeks have been difficult and I would be quite lost and utterly overwhelmed with everything if I hadn’t got your help.”
In preparation, a baseline assessment of our helpline was carried out through a more detailed (than normal) audit of the NRAS helpline service, which began at the end of 2018 and is on-going.
Currently 224 responses have been analysed. In the audit:
- 78% scored their level of concern about their disease at 7 or higher out of 10
- only 8% scored 5 or below
When asked about the effects of their RA on emotional wellbeing:
- 62% scored it as 7 or more where 10 was the worst possible impact
- 94% said that they would definitely, or very likely, recommend NRAS and its services to another person.
These results led ultimately to the development of the Right Start service, launched in 2019, whereby health professionals across the UK can refer their patients directly to NRAS for a targeted intervention via a consented online referral - fully GDPR compliant.
Before we created ‘Right Start’, an Advisory Board comprising 7 clinicians, from 7 rheumatology units was appointed to work with NRAS on this research which initially was a ‘Quality Improvement Programme’ pilot in the 7 units. We believed that it would:
- Meet the needs of their newly diagnosed patients
- Improve their service delivery outcomes
- Enable compliance with national audit requirements
Resulting in:
- Improved efficiency of the unit (ease of referral and ensuring patients receive education and self-management per QS33 Std. 3)
- Cost saving (by increasing self-efficacy of patients and thereby reducing use of valuable NHS resources)
- improved patient outcomes
We are a national organisation covering the whole of the UK and we are addressing the needs of the >400,000 people living with RA and the 12-15,000 children and young people living with JIA.
How did you implement the project
At the time we were developing Right Start, Ailsa Bosworth MBE, our National Patient Champion, was on the Expert Group revising QS33 in line with NG100. It made complete sense to ensure that Right Start enabled HCPs to meet Statement 3 in both the old and the new Quality Standard on patient education and provision of supported self-management.
The seven consultant rheumatologists with whom we were working on the development of Right Start to effectively enable us to ‘demonstrate the value of NRAS’ were in complete agreement about alignment with NICE Quality Standards. We had no difficulty with buy-in from any of our stakeholders, including people with RA we spoke to about the proposal.
When we triggered the start of referrals from these 7 rheumatology units, as the initial pilot, we found that we met data protection issues from a number, in spite of the enthusiastic support of the consultants involved. In order to resolve this in a consented and compliant way, we developed the Quality Improvement Programme pilot into a ‘Service’ and created an online referral form (much like MacMillan’s on-line referral) which HCPs could use to refer patients easily in a consented way which met their and our GDPR standards. We developed relevant supportive materials and resources for use by patients and HCPs including a patient leaflet, a poster and an HCP reference resource and launched the service at the BSR congress 2019. The service was met with enthusiastic support from all the HCPs (over 300) we spoke to at the congress.
The costs of developing the service primarily relate to our time (our most precious resource!) and in that respect have run into the many thousands as the initial idea for this service started over 2.5 years ago). In addition, there are direct costs of the resources to promote the service, described above. This amounts to design and print costs of approx.£2,000 in 2019. We have budgeted further costs for promotion of the service in 2020 and also expansion by developing a similar, new service called ‘Living Better with RA’ for those with existing disease. All these costs have been borne by NRAS out of existing funds. This is a key and priority piece of work for us.
Key findings
The initial results of our service have been overwhelmingly positive and encouraging from both HCPs and patients. To date (as at early Feb 2020), we have 25 referring hospitals and have had over 100 newly diagnosed patients referred to us. See chart below:
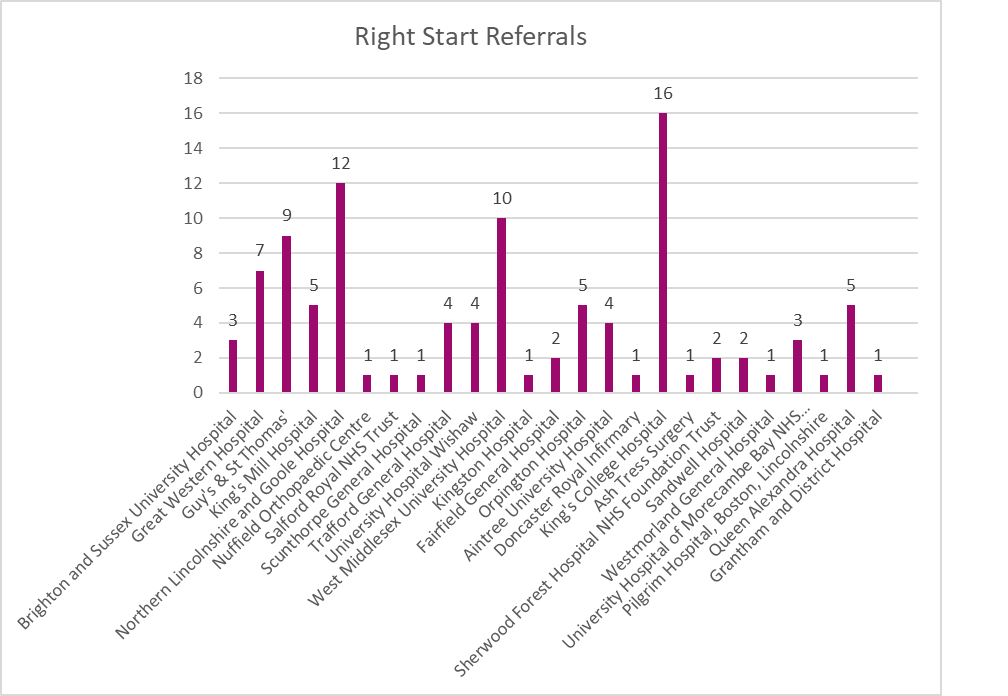
The call/intervention status on each of the referrals is as follows:
|
Total open calls |
10 |
|
Total successfully closed calls |
58 |
|
Total closed calls no contact |
34 |
|
Total calls |
102 |
Where we are unable to get a response from a referred person (either by phone or email), after we have tried 3 times, we forward a newly diagnosed pack with a letter to ensure that they have the basic information they need. The pack includes 3 booklets: Newly Diagnosed, Medicines in RA and Fatigue Matters, and are encouraged to call us for further help. We are targeting to significantly increase the number of referring hospitals and patients referred in 2020 and will be again using the BSR congress in Glasgow at the end of April to promote the service.
A Nurse Consultant (West Middx. and Chelsea/Westminster) said of the service:
“I have found Right Start to be an excellent resource for people who have recently been diagnosed with RA. When time is limited time in clinic, a referral provides the patient with tailored information which complements the education I have been able to provide. Feedback from patients has been positive particularly relating to the phone calls with the NRAS helpline team and the NRAS volunteer with RA. It is I would definitely recommend the service.”
Dr James Galloway, Senior Lecturer & Honorary Consultant at King’s, who is also the Data Lead for the NEIAA, is doing the analysis of all the data collected as part of Right Start. As new patients get entered into the National Audit, they are asked to complete a PROM, the MSKHQ, at baseline and again at 3 months. Those who are referred to NRAS Right Start at point of diagnosis will have therefore completed this PROM. Prior to their follow up visit and repeat PROM at 3 months, they will have received the Right Start service and these patients’ outcomes are being compared to patients in the Audit who have not yet had access to Right Start.
Feedback from HCPs as above, tells us that this service is saving time for the nurses who generally provide education. Anecdotal feedback from patients is overwhelmingly positive. We await data analysis from King’s which should be available on the first 50-100 patients within the next 2-3 months.
Key learning points
Doing a rigorous audit of our helpline (as a key component of Right Start service) was a critical starting point for this work using a validated questionnaire recommended by Dr Galloway so that we could demonstrate successfully that this was a beneficial and valued service for people with RA. We continue to audit a small number of people against the same criteria to ensure that our service standards remain consistently high.
We could have saved time had we developed the ‘service’ idea with consented on-line referral earlier, as we did have issues with various IT departments amongst the 7 hospitals who originally signed up to the pilot of the Quality Improvement Programme. However, once this was all in place, hospital sign-ups increased significantly, and the issues went away.
In addition to reducing the burden on health professionals who have less time and resource at their disposal than used to be the case, and improving patient outcomes, we hope this work will help to demonstrate not only our value as an expert patient organisation, but the value of patient organisations more broadly.
This work also dovetails well with a EULAR research study Ailsa Bosworth is the lead convenor on entitled: EULAR Recommendations for the implementation of self-management strategies in patients with Inflammatory Arthritis (IA). The background to this EULAR study is that an important aspect of care in IA is the ability to understand the disease and deal with the practical, physical and psychological impacts that come along with it. This goes beyond drug therapy and recognises that the diagnosis of IA is life-changing and the ability to self-manage, an essential component of care. Objectives are to develop pan-European EULAR recommendations for the implementation of effective self-management strategies in IA concurrently with standard medical care for Health Professionals so that the routine outpatient clinic appointments become more holistically focussed beyond the purely clinical/medical.