Overview
This guideline covers preventing bacterial infection in healthy babies of up to and including 28 days corrected gestational age, treating pregnant women and pregnant trans men and non-binary people whose unborn baby is at risk of infection, and caring for babies of up to and including 28 days corrected gestational age with a suspected or confirmed bacterial infection. It aims to reduce delays in recognising and treating infection and prevent unnecessary use of antibiotics. The guideline does not cover viral infections.
Where the term 'parents' is used, this should be taken to include anyone who has main responsibility for caring for a baby. We recognise there are many different family arrangements.
Last reviewed: 13 May 2026
We have reviewed the evidence on the time between prelabour rupture of membranes and birth (at term) to see if this affects the risk of early-onset neonatal infection. We have also amended the risk factors related to fever and chorioamnionitis because of safety concerns. See box 1 on risk factors for early-onset infection.
We have reviewed the evidence on switching from intravenous to oral antibiotics when treating suspected early-onset neonatal infection. New recommendations are marked as [2026]. See the section on switching to oral antibiotics for early-onset infection.
See update information for more details.
This guideline updates and replaces NICE guideline CG149 (August 2012).
Next review: This guideline will be reviewed if there is new evidence that is likely to change the recommendations
How we prioritise updating our guidance
Decisions about updating our guidance are made by NICE’s prioritisation board. For more information on the principles and process, see NICE-wide topic prioritisation: the manual.
For information about individual topics, including any decisions affecting this guideline, see the summary table of prioritisation board decisions.
Recommendations
This guideline includes recommendations on:
- prevention and risk reduction
- risk factors and clinical indicators: early-onset neonatal infection
- risk factors and clinical indicators: late-onset neonatal infection
- principles around use of antibiotics
- antibiotics for early-onset neonatal infection
- antibiotics for late-onset neonatal infection
- meningitis
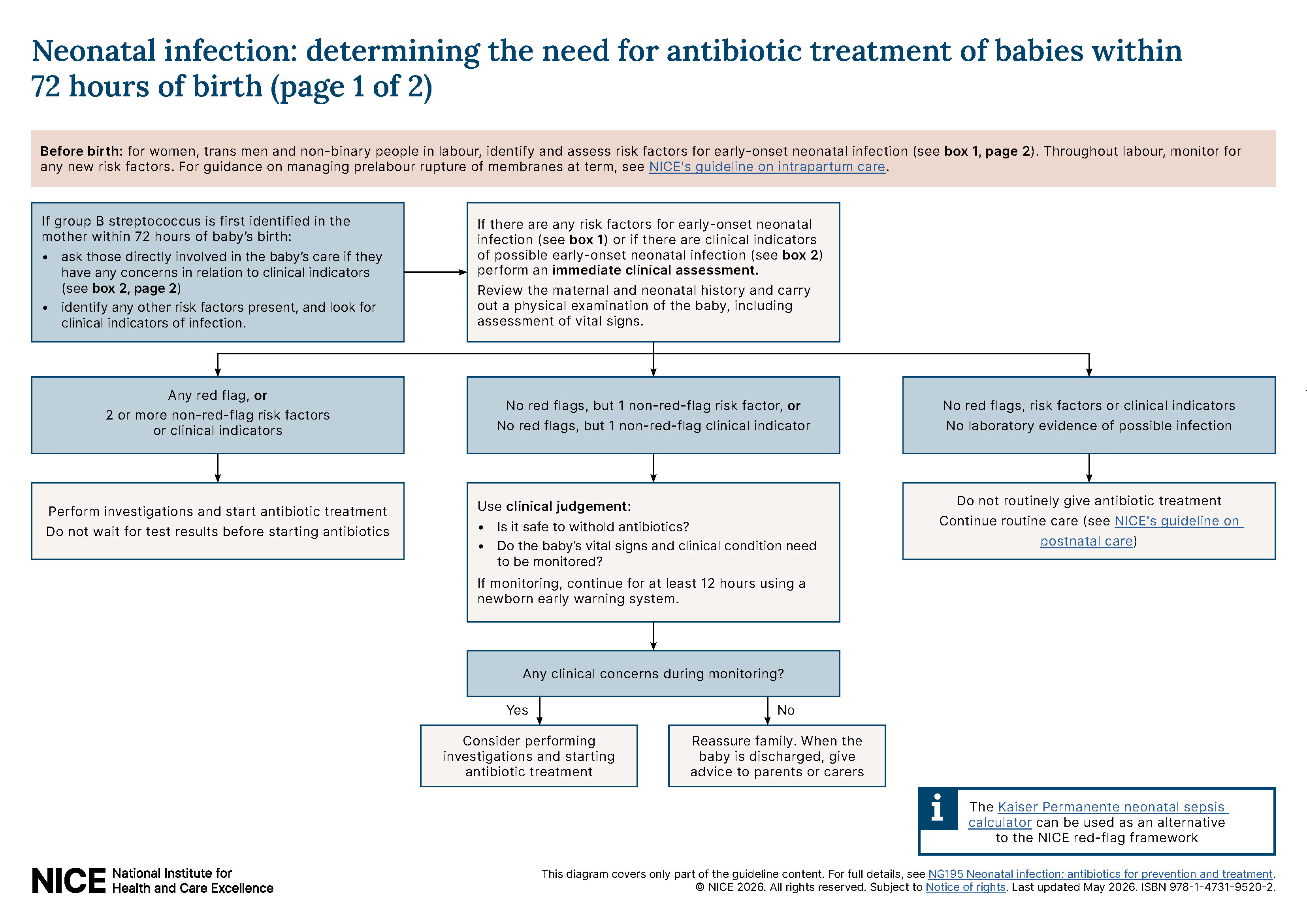
See the visual summaries on the recommendations for determining the need for antibiotic treatment of babies within 72 hours of birth and duration of antibiotic treatment for late-onset neonatal infection without meningitis.
Who is it for?
- Healthcare professionals in primary and secondary care
- Commissioners and providers of neonatal and maternity services
- Parents and carers of babies who are at risk of or who have a neonatal infection
Guideline development process
How we develop NICE guidelines
This guideline was commissioned by NICE and developed in partnership with the Royal College of Obstetricians and Gynaecologists (RCOG)
Your responsibility
The recommendations in this guideline represent the view of NICE, arrived at after careful consideration of the evidence available. When exercising their judgement, professionals and practitioners are expected to take this guideline fully into account, alongside the individual needs, preferences and values of their patients or the people using their service. It is not mandatory to apply the recommendations, and the guideline does not override the responsibility to make decisions appropriate to the circumstances of the individual, in consultation with them and their families and carers or guardian.
All problems (adverse events) related to a medicine or medical device used for treatment or in a procedure should be reported to the Medicines and Healthcare products Regulatory Agency using the Yellow Card Scheme.
Local commissioners and providers of healthcare have a responsibility to enable the guideline to be applied when individual professionals and people using services wish to use it. They should do so in the context of local and national priorities for funding and developing services, and in light of their duties to have due regard to the need to eliminate unlawful discrimination, to advance equality of opportunity and to reduce health inequalities. Nothing in this guideline should be interpreted in a way that would be inconsistent with complying with those duties.
Commissioners and providers have a responsibility to promote an environmentally sustainable health and care system and should assess and reduce the environmental impact of implementing NICE recommendations wherever possible.