More than 20,000 people benefitting from innovative migraine pills recommended by NICE
A new type of tablet specifically designed to prevent migraine is transforming lives across England, with the number of people being prescribed these medicines more than tripling in just one year.

NICE’s approval of the therapies has given people with migraine further treatment choice.
Joanne McShane, an NHS health visitor, had suffered from migraine for a decade when she was first prescribed atogepant in 2024, shortly after NICE recommended the new treatment option.
“It is life changing,” she said. “I thought ‘this is going to be another thing that works for a little while and then stops’. But I haven't had a headache since. It has restored my life.”
In 2025, 22,800 people were prescribed atogepant or rimegepant by their GPs – more than triple the number in 2024 – following NICE approval of the treatments. The total receiving these tablets across the NHS is higher still, as these figures exclude prescriptions from hospitals and specialist clinics.
NICE's approval of these new tablets has widened access for those whom other preventive therapies had failed.
A common but misunderstood condition
Around one in seven people in the UK live with migraine. “It is nearly as common as asthma, epilepsy, and diabetes combined,” says Rob Music, chief executive at The Migraine Trust.
A migraine is not the same as a headache. Symptoms can include severe throbbing pain, nausea, vomiting, tiredness, and extreme sensitivity to light, sounds and smells. Attacks can last for days and are more common in women than men.
The impact extends beyond individual suffering. Migraine causes millions of lost workdays every year, costing the UK economy more than £4 billion. Research undertaken for The Migraine Trust puts the figure at around £9 billion a year when accounting for presenteeism – people at work but unable to perform at their best.
Joanne used to have around six migraine attacks per month. “It could take three days for the pain to subside and get out of that exhaustion before I would get another attack, so I didn’t get much time in between,” she said. “It affected my driving, my ability to work and just to interact with people. I couldn’t even plan to go out with friends. You can become very isolated.”
A Migraine Trust survey of 2,000 people found 89% said the condition had affected their mental health, and a third reported having thoughts of suicide due to their migraine.
“Many feel they are not believed, there’s a stigma associated with it, and on top of that there’s the struggle to get onto the right care pathway as quickly as possible,” Rob said.
Why these tablets are different
Until recently, preventive treatments included antidepressants, antiepileptics and beta-blockers. These medicines are not designed specifically for migraine and often come with difficult side effects or contraindications, or stop working over time.
Atogepant and rimegepant block CGRP (calcitonin gene-related peptide), a chemical associated with migraine attacks. Although CGRP-targeting therapies have been available for several years as infusions or injections, these are the first that can be taken as tablets.
“There are some people who are unable to tolerate or have issues with injections for whom an oral option is much easier,” said Rob. “There's also an opportunity for them to be offered in primary care and that's better not only for the patient, but for the NHS given the current capacity challenges.”
NICE recommended rimegepant in 2023 for treating migraine and preventing episodic attacks (between 4 and 14 migraines per month), and atogepant in 2024 for preventing both episodic and chronic migraine (15 or more headache days per month). The pills can be used by adults to prevent migraine if at least three other preventive treatments have failed.
Rapid uptake across the NHS
In 2025, 22,800 people were prescribed at least one of these tablets by their GP. Some people were prescribed both treatments during the year – around 14,500 received rimegepant and 9,300 atogepant.
Figure 1: Number of people prescribed atogepant or rimegepant in primary care in England
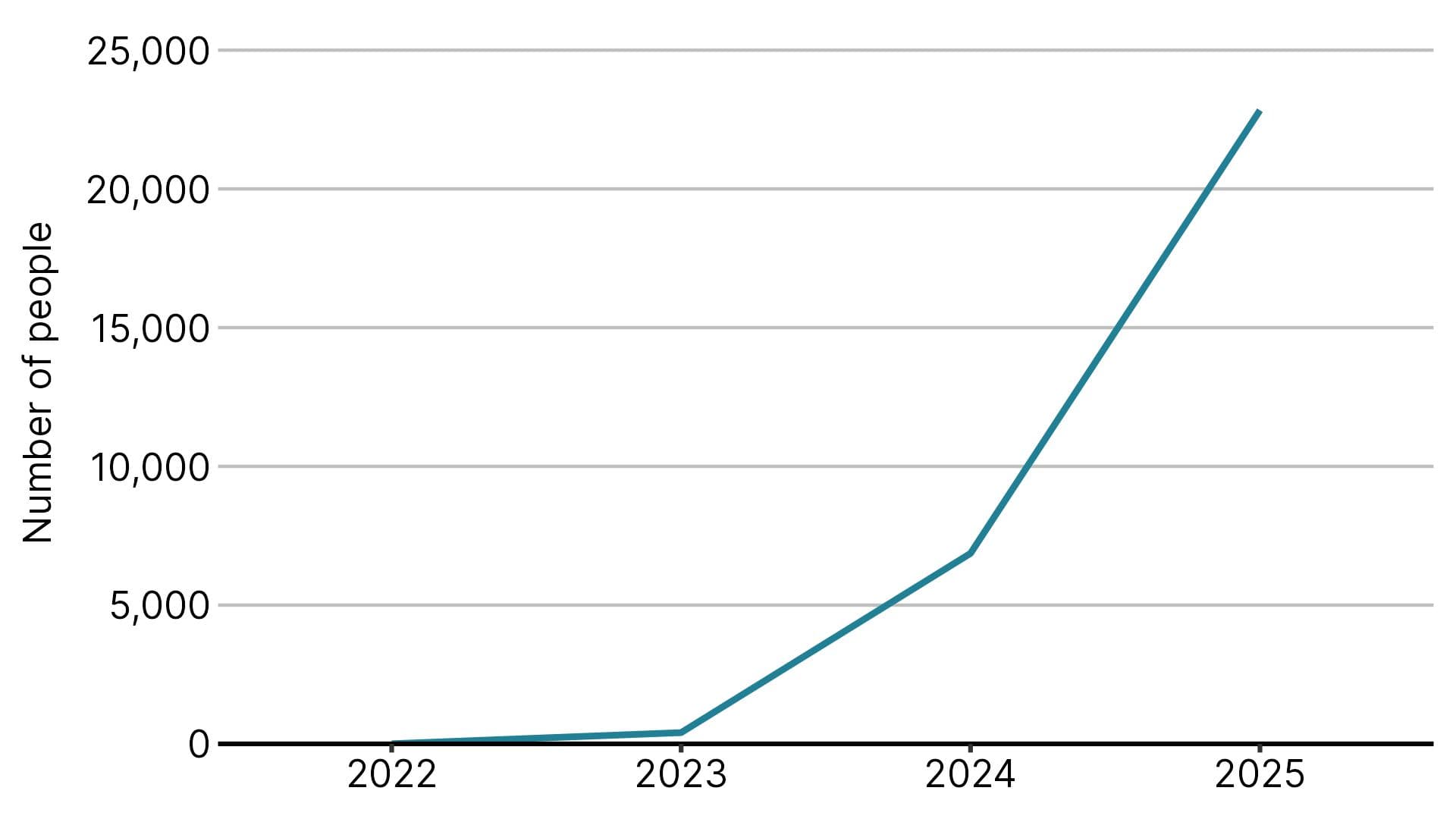
Source: NICE analysis of NHSBSA data
Overall use of these tablets, including in hospitals and specialist clinics, has also risen sharply.
Figure 2: Usage of atogepant and rimegepant in England, by month
Total volume across primary and secondary care
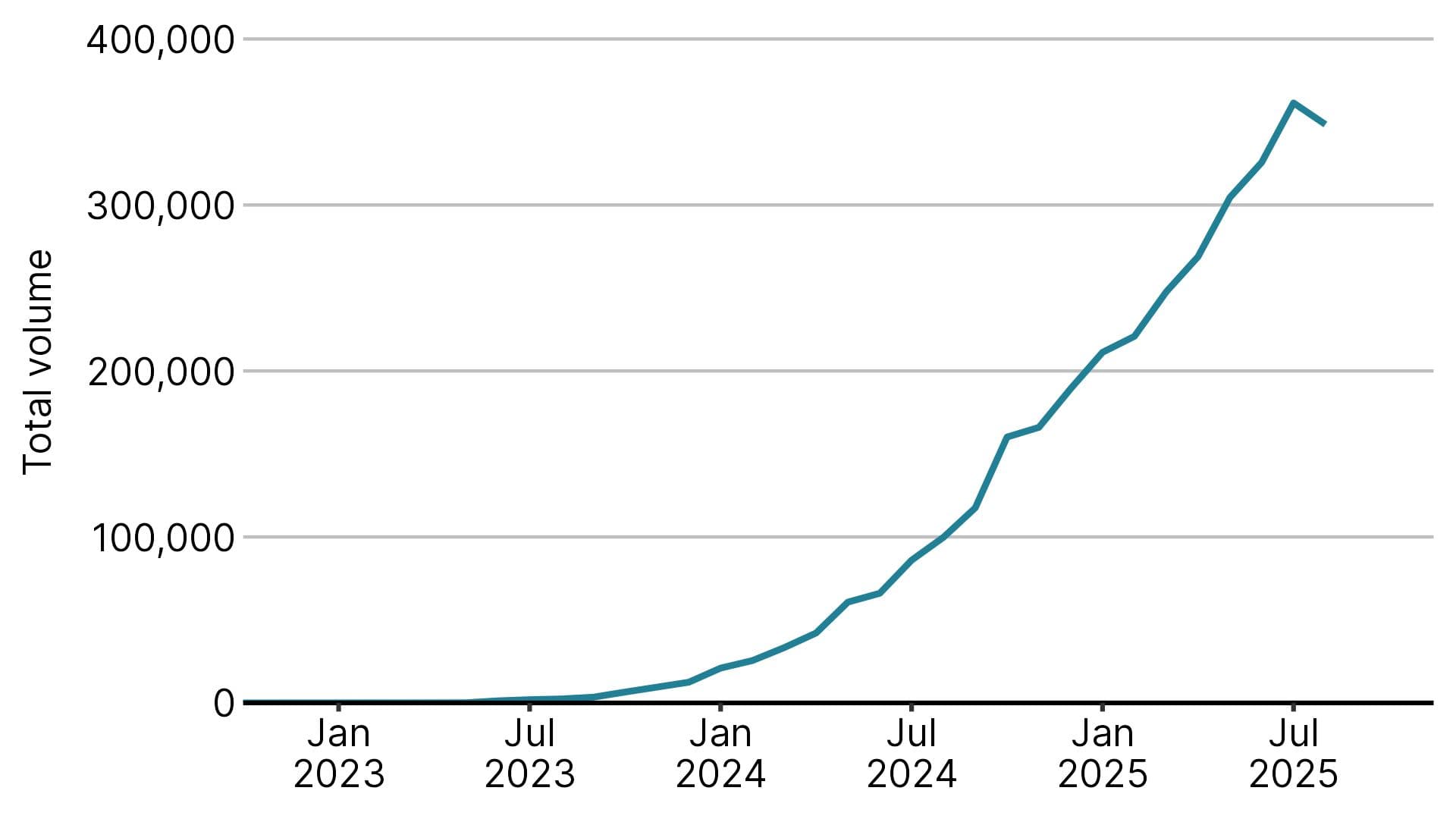
Figures up to Aug 2025. Data is in DDD (Defined Daily Dose). This is the assumed average daily dose for a drug used for its main indication in adults. Source: NICE analysis of RXinfo Define data.
Dr Kay Kennis, GP with an extended role in Headache at Bradford Community Neurology Service said:
"There were many people who had already tried three traditional preventers to maximum tolerated doses for three months each and specialists had nothing else to offer them. They were all ready to start these tablets."
She added that the new treatments – all the CGRP targeting therapies, including the injectables – have been transformative: "We can now make a significant difference to the lives of many more patients who live with migraine, offering them real improvements in their quality of life and ability to continue working, studying or looking after their family."
Challenges remain
For patients who haven't exhausted other preventive options, waiting times can be long, as the tablets usually need to be initiated by specialists. There are also regional disparities in access, and some patients do not respond to these therapies – leaving them still waiting for new treatment options.
Cost is another consideration. "The difficulty for the NHS is the price of these medications," Dr Kennis said. "They do need to be prescribed appropriately, otherwise it's a waste of resources."
Experts suggest that greater focus on 'green flags' - signs in the clinical history that indicate a patient has migraine rather than another condition - could give GPs confidence to prescribe treatments earlier. This would help patients move through first-line preventers faster and access specialist options like atogepant and rimegepant if needed.
These tablets are already transforming the lives of thousands of people with migraine in England, and the rapid uptake is very encouraging. NICE is committed to helping get the best care to patients and ensure clinically and cost-effective medicines are available to those who need them. We hope this continued momentum means even more people can benefit in the months ahead.